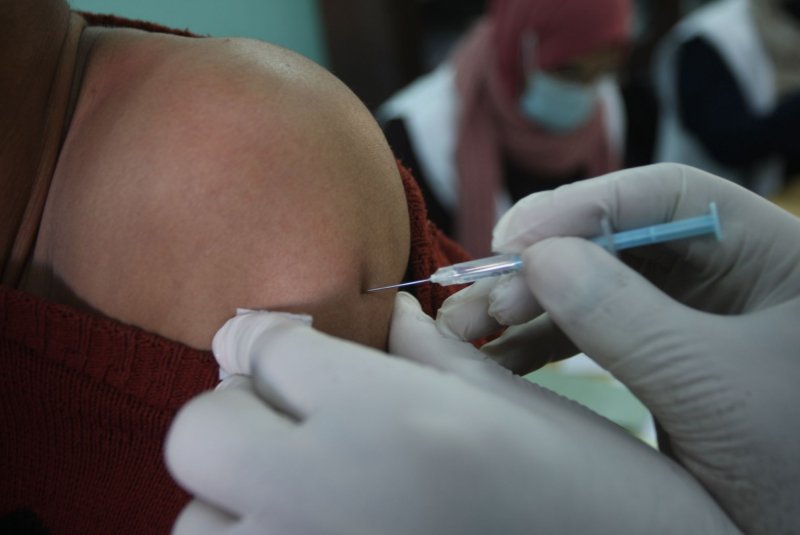
Researchers at the UPMC Hillman Cancer Center are exploring a groundbreaking method for treating early-stage breast cancer by delivering radiation therapy before surgery. This innovative clinical trial, led by assistant professors Dr. Parul Barry and Dr. Ravi Patel from the University of Pittsburgh, aims to shrink tumors using targeted doses of radiation prior to surgical intervention.
Traditionally, breast cancer patients undergo radiation treatment after surgery, typically spanning three to seven weeks. This lengthy schedule often discourages women from completing necessary treatment, particularly those managing work or caregiving responsibilities. According to Dr. Barry, approximately one-third of patients in the United States do not finish their radiation therapy. In contrast, the Hillman trial simplifies this process by administering just five radiation treatments over the course of about one week, effectively reducing the total treatment duration to around three weeks.
The objective is clear: to minimize side effects, shorten treatment times, and potentially eliminate the need for surgery altogether in the future. “With just five treatments and relatively low toxicity, you’re kind of mitigating some of the reasons why people may skip radiation,” Barry noted. “People fly through the treatment and do well and tolerate it well.”
Emerging research from Dr. Patel’s lab suggests that pre-surgery radiation could also enhance the body’s immune response to cancer. “When we irradiate the tumor, we can cause some of those cancer cells to die and release what we call cancer neoantigens that your immune system can process,” he explained. “We can potentially mount an immune response against cancer if we give the radiation upfront, rather than after surgery.”
Collaboration between clinicians and scientists is a hallmark of this trial. Blood samples from each patient are quickly analyzed in Patel’s lab for immune markers and molecular responses to the treatment. This real-time data collection could help identify which patients are most likely to benefit from the approach, and possibly those who could forgo surgery entirely in the future. “This is truly a bench-to-bedside trial,” Barry stated. “That’s the only way we’ll actually be able to move precision therapy forward.”
Dr. Margaret Quinn Rosenzweig, an oncology nurse-researcher at Pittsburgh, emphasized the significance of patient confidence in clinical trials. She noted that patients often seek reassurance from their physicians regarding participation. “Is this something you would recommend for me? And is this something you would do for your own family?” are common queries, highlighting the importance of trust in medical recommendations.
Rosenzweig pointed out that trials like Barry’s are notable because they arise from clinicians addressing concerns encountered in everyday practice. “It’s a brave clinician who’s questioning their own practice,” she remarked. “It’s really a true scientist who will say, are we doing everything in exactly the way we should be or could we change this?”
The concept of administering radiation before surgery is not novel; it has become standard in the treatment of colorectal cancer and is increasingly being investigated for other cancers. By shrinking tumors prior to surgery, this method may reduce the need for more invasive procedures and help preserve organ function. Barry noted promising preliminary results, stating, “Overall, [the breasts] look almost as normal as they did before surgery. People are flying through this radiation and healing very, very well. The toxicity is very, very low.”
This approach could significantly impact the psychosocial well-being of women facing breast cancer, as Barry stressed the importance of preserving the breast. “A lot of what radiation allows for is organ preservation,” she said. “For women, breasts are so important psychosocially. Radiation allows people to still get cancer cure without too much disfigurement.”
Currently, the trial is enrolling patients with stage 1 hormone-sensitive breast cancers and aims to expand to include individuals with higher-risk cancers and explore new combinations of radiation with chemotherapy or hormone therapy. As this research progresses, it holds the potential to transform breast cancer treatment, making it more effective and less burdensome for patients.